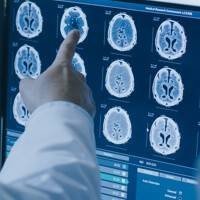
The brain is an important organ of the human body that controls our thinking, memory, language, emotion, and movement abilities. When the brain is invaded by cancer cells, its function will be affected to varying degrees. Despite the common perception that all brain tumors are malignant, they can actually be benign. The difference between the two lies in the tumors’ speed of growth, the degree of their manifestation in the brain, and the recurrence rate. In addition, brain tumors can also be categorized into ‘brain cancer metastasis (secondary)’ and ‘primary brain tumors (non-metastatic)’.
Classification of Brain Tumors
| Benign brain tumors | Glioma, meningioma, oligodendroglioma, schwannoma, pituitary adenoma, brain cyst, etc. |
|
Malignant brain tumors |
Metastatic brain tumors, glioblastoma (GBM), brain lymphoma, craniopharyngioma, hemangioblastoma, etc. |
|
Primary brain tumors |
80% of tumors originating from cells in the brain are gliomas. |
|
Brain cancer metastasis (secondary) |
|
Symptoms of brain tumors
The human skull is hard and has no flexibility. Therefore, regardless of the nature of the brain tumor – whether it is benign or malignant – once it grows to a certain size, brain tissue will be compressed which will cause growing pressure inside the skull. Depending on the location of the tumor, the following symptoms may appear:
- Frequent and severe headaches
- Difficulty with balance and walking
- Seizures
- Unexplained nausea or vomiting
- Vision problems, such as blurred vision, double vision or loss of vision
- Hearing problems
What are brain metastases?
Brain metastases refer to the condition when the cancer cells that start from one place in the body spread to the brain, which is also called secondary brain cancer and it is the last stage. Although the prognosis of patients with untreated brain metastases is only 1 to 3 months, it does not mean there is no cure. If brain tumors are left to grow, the symptoms could drastically affect the patient’s quality of life and would also hinder the control of cancer in situ. Currently, there are various ways to treat brain metastases including brain surgery, radiation therapy, and drug therapy.
Various treatment methods to increase patients' survival rate
Since treatments for brain tumors are restricted by the brain’s blood-brain barrier (BBB) mechanism, it is difficult for most targeted therapy and traditional chemotherapy to go through the barrier and work their way to the brain, which often results in unsatisfactory treatment outcomes. That is the reason why the main effective treatment methods for brain cancer are surgery and radiotherapy.
1. Brain surgery
Applicable to patients with:
-
- Only 1-4 metastatic brain lesions with stable health conditions and their primary cancer is under control. If the patient does not have a lot of tumors in the brain, surgery can remove all tumors in one go.
- Brain tumors having a diameter larger than 2-3 cm. This could increase the patient’s intracranial pressure, posing an immediate life threat to the patient. Surgery is required immediately to save the patient’s life.
- Brain tumors with an unknown nature. Pathological tests will be performed after the removal of the tumor to help the doctor determine the next step in the treatment plan.
However, resection of brain tumors is a relatively traumatic treatment option. Some patients may have some remaining brain tumor cells left in the brain after the surgery, hence adjuvant radiotherapy is required to reduce the risk of recurrence.
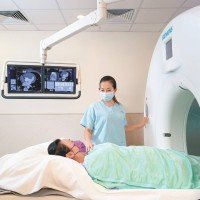
2. Radiotherapy
Radiotherapy can be classified into whole-brain radiotherapy (WBRT) and stereotactic radiotherapy (SRT).
| Whole-brain radiotherapy (WBRT) | Whole-brain radiotherapy (WBRT) | |
|
Process |
|
|
|
Effectiveness |
It helps reduce the risk of recurrence and improve the overall survival rate of patients |
Brain tissue that is not within the scope of radiotherapy may have a relatively high recurrence rate. |
|
Patients applicable |
Patients with more than 10 metastatic brain lesions |
|
|
Side effects |
It causes more damage to the brain tissue and brings more side effects. For example, some patients may have problems with their memory after the treatment. |
Stereotactic radiotherapy is a type of targeted therapy, hence the side effects are significantly reduced. Patients may experience partial hair loss, but in general, their cognitive ability and memory will not be affected. |
Common Brain Tumor - Glioma
- The human brain has billions of cells and 90% of which are glial cells, whose function is to support the functioning of nerve cells. However, when they mutate, they will turn into gliomas.
- Gliomas are very common, accounting for about 30% of all nerve tumors which can be benign or malignant. Glioblastoma multiforme (GBM) is a type of malignant tumor. It grows fast and has a high recurrence rate. Patients often only have an average survival period of 15 months, and the age of onset is generally between 40 and 60 years old.
- Gliomas can appear anywhere in the brain, and the symptoms depend on the location. Common symptoms are similar to that of other brain tumors, but patients may experience cramps, weakness of hands and feet, paralysis, and changes in thoughts and behaviors.
Treatment methods
A brand new treatment option: Tumor Treating Fields (TTFields) combined with standard treatments (which includes surgery, radiotherapy, chemotherapy, and drug therapy) to treat glioblastoma cells (GBM)
The standard treatment for GBM is oral chemotherapy for 6 to 12 months after surgery and concurrent radiotherapy and chemotherapy. However, the recurrence rate is often still high. The latest clinical studies have confirmed that concurrent TTFields and oral chemotherapy can effectively prolong the survival period of patients.
Tumor Treating Fields (TTFields) interfere with cancer cell division
- Electric fields interfere with cancer cells: TTFields are a biophysical treatment method that delivers alternating electric fields of specific frequencies to the lesions through the electrode stickers that are attached to the skin. The electric fields interfere with the division of cancer cells, thereby controlling their growth and even leading to their apoptosis.
- The effect of long-term wear is ideal: The TTfields treatment device is portable and will not affect the patient's daily routine. During the treatment, patients can leave home, do chores or even do light exercises whilst wearing the device. For the treatment to be effective, patients need to wear the device for at least 18 hours a day. The longer the patients wear the device, the better the treatment effect.
- Safe and effective: This treatment works by creating electric fields that disrupt cancer cell division. It is proven safe and electric shocks rarely happen if used properly.
- Few side effects: Only a small number of patients may experience redness and itching on the scalp due to long-term wear of the device, and this can be effectively treated with ointment prescribed by doctors.
Effectively prolong the life expectancy of patients with GBM
- Approved by FDA: TTFields have been approved by the U.S. Food and Drug Administration (FDA) as a treatment for newly diagnosed and recurrent GBM. According to a large-scale phase III clinical study on patients with first diagnosis of GBM, their life expectancy is increased from 16 months (taking the approach of concurrent radiotherapy and chemotherapy) to 21 months after undergoing surgery, concurrent radiotherapy and chemotherapy, as well as taking an oral chemotherapeutic drug named 'Temozolomide' combining the treatment of TTfields.
- Fewer side effects: As for recurrent GBM cases, another phase III clinical study showed that the therapeutic effect of TTfields alone is similar to that of second-line chemotherapy, but there are fewer side effects compared with traditional chemotherapy. Under the treatment of TTfields, patients will be able to have better quality of life, hence they are more accepting of this treatment method.