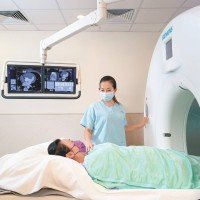
Understanding Breast Cancer: Symptoms, Causes, and High-Risk Groups
1 in every 14 women in Hong Kong is at risk of developing breast cancer during her lifetime. Over 94% of breast cancer patients are aged 40 or above, and the risk increases with age. In 2022, breast cancer surpassed colorectal cancer to become the second most common cancer in Hong Kong. Early detection significantly improves treatment outcomes and survival rates
What is Breast Cancer?
Cancer occurs when abnormal cells grow uncontrollably, damaging healthy tissues and spreading to other organs. When a malignant tumor develops in the breast, the most common type is breast cancer, which may spread within the breast and to other parts of the body.
Symptoms of Breast Cancer
- Presence of a lump or changes in breast shape
- Dimpling of the skin (like a dimple), orange peel texture, or visible vein enlargement on the breast
- Nipple bleeding or inversion
- Swelling or lump in the underarm lymph nodes
High-Risk Groups for Breast Cancer
- Older Age: According to the Hong Kong Cancer Registry’s data from 2020 to 2022, over 70% of newly diagnosed breast cancer cases occurred in women aged 50 or above.
- Unhealthy Lifestyle: Risk factors include obesity, lack of exercise, alcohol consumption, smoking, frequent intake of high-fat foods, and long-term use of birth control pills or hormone replacement therapy for more than 5 years.
- Genetics: Studies show that women with a amily history of breast cancer in first-degree relative have a higher risk compared to those without.
Causes of Breast Cancer
The exact cause of breast cancer remains uncertain. However, various risk factors—such as a family history of breast cancer—are associated with higher chance of developing breast cancer. Our hospital encourages women to undergo regular breast examinations, including self-checks, clinical breast exams, and mammography. By staying alert to changes in the breasts and adopting a three-pronged screening approach, early detection becomes possible, allowing for effective treatment.
|
Non-Modifiable Risk Factors |
Modifiable Risk Factors |
|
Age |
Never given birth, or having the first childbirth after age 35 |
|
Family history of breast cancer |
Never breastfed |
|
Genetic predisposition |
Undergoing hormone replacement therapy |
|
Early onset of menstruation or late menopause |
Received chest radiation therapy before age 30 |
|
Personal history of breast cancer |
Overweight or obese after menopause |
|
History of benign breast disease |
Alcohol consumption |
|
|
Lack of physical activity |
Breast Screening Guidelines for Women (Without Symptoms) + How Breast Cancer Is Diagnosed
If you have a family history of breast cancer or other high-risk factors, consult your doctor first.
| Monthly breast self-examination | Mammogram every two years | |
| 20-39 years old | ✓ | |
| 40-49 years old | ✓ | ✓ |
| 50-69 years old | ✓ | ✓ |
Breast Examination Methods and Diagnostic Process
It is recommended that women aged 20 and above perform regular monthly breast self-examinations. For those who have not yet reached menopause, the examination should be conducted on the 7th to 10th day after the start of menstruation. For postmenopausal women, the examination should be performed on the same day each month.
- Observation
Stand in front of a mirror with your arms raised above your head. Observe whether there are any abnormalities such as changes in the skin and nipple, or discharge. Place your palms on your hips and press down firmly to tighten the chest muscles, and check if there is any dimpling or indentation of the breasts. - Comparison
Compare both breasts carefully, noting whether there are any unusual differences in size or shape. Pay attention to the overall contour, skin texture, or outline of the breasts, and see if they look different from what you are familiar with in the past. - Palpation (Touch)
Raise your right arm and place it behind your head. Use the flat pads of the middle three fingers of your left hand to make small circular motions over the right breast, moving from the outer side inward toward the nipple. Gently squeeze the right nipple to check for any discharge. Switch hands and repeat the same method to examine the left breast, nipple, and armpit for any lumps, swelling, or hardness.
How is Breast Cancer Diagnosed?
Clinical Examination
A specialist doctor performs a physical examination of the breasts to check for abnormalities, such as lumps or nipple discharge, and then determines whether further tests like mammography or ultrasound are needed.
Mammography
Mammography uses X-ray imaging of the breasts to detect abnormal tissue or tumors that cannot be felt or are not yet formed. It is particularly useful for identifying early-stage breast cancer.
Ultrasound Scan
Ultrasound helps distinguish the location, size, and type of breast lumps.
Magnetic Resonance Imaging (MRI)
In certain circumstances, MRI provides a more detailed evaluation of abnormal areas in the breast.
Biopsy (Needle Aspiration Test)
Also known as a breast needle biopsy, this procedure involves using a fine needle to extract tissue from a lump, as recommended by the doctor, to determine the type of cells present.
Recommended Groups for Regular Breast Examinations
- Women aged 20 to 40 should have a breast examination by a doctor every 3 years.
- Women aged 40 and above should have a breast examination by a doctor and undergo mammography every 2 years.
- Women with close relatives who have had breast cancer should have a breast examination by a doctor and undergo mammography once a year.
Types of Breast Cancer and Pathological Analysis
| Types of Breast Cancer | Pathological Analysis |
| Ductal Carcinoma In Situ (DCIS) | The cancer cells remain confined within the milk ducts and have not invaded surrounding breast tissue. It is considered a very early stage of breast cancer. |
| Invasive Ductal Carcinoma (IDC) | This is the most common type of breast cancer, accounting for about 80% of invasive cases. The cancer cells have penetrated the wall of the milk ducts and invaded the fatty tissue of the breast, requiring timely treatment. |
| Invasive Lobular Carcinoma (ILC) | This type of breast cancer originates in the lobules of the breast and requires timely treatment to prevent spreading. Because it is more difficult to detect through mammography, magnetic resonance imaging (MRI) is often used as an additional diagnostic tool. |
| Luminal Breast Cancer | This is a hormone‑dependent type of breast cancer. It is characterized by hormone receptor positivity and HER2 receptor negativity (HR+, HER2–). It is also commonly referred to as luminal hormone‑positive breast cancer. |
|
HER2-Positive Breast Cancer |
HER2-positive breast cancer is considered more aggressive, but with modern targeted therapies, patient survival has improved. |
| Triple-Negative Breast Cancer (TNBC) | Triple-negative breast cancer accounts for about 10–15% of all breast cancer cases. It is more commonly seen in younger women and in hereditary breast cancer associated with the BRCA1 gene. This type is characterized by a higher tendency to spread to other organs and a greater risk of recurrence. |
Breast Cancer Stages + Treatment
Staging of breast cancer is a key factor in determining treatment plans and predicting patient survival (prognosis). Doctors generally use the internationally recognized TNM staging system to assess the extent of cancer spread. The TNM system takes into account three core indicators: tumor size (T), lymph node involvement (N), and distant metastasis (M).
Tumor Size (T) Classification
This indicator evaluates the size of the primary tumor and whether it has invaded the chest wall or skin.
| T Classification | Description |
| T0 | No evidence of tumor. |
| Tis | Ductal Carcinoma In Situ (DCIS): Cancer cells are confined within the milk ducts of the breast and have not invaded the basement membrane. |
| T1 | Maximum tumor diameter ≤ 2 cm. |
| T2 | Maximum tumor diameter >2 cm but ≤5 cm. |
| T3 | Maximum tumor diameter >5 cm. |
| T4 | Tumor of any size with direct invasion of the chest wall or skin (such as ulceration or edema). |
Lymph Node (N) Metastasis Status
This indicator assesses whether cancer cells have spread to nearby lymph nodes, typically the axillary lymph nodes.
| N Classification | Description |
| N0 | No evidence of lymph node metastasis. |
| N1 | Cancer cells have spread to 1 to 3 ipsilateral (same side) axillary lymph nodes. |
| N2 | Cancer cells have spread to 4 to 9 ipsilateral axillary lymph nodes. |
| N3 | Cancer cells have spread to 10 or more ipsilateral axillary lymph nodes, or to infraclavicular/supraclavicular lymph nodes. |
Distant Metastasis (M) Status
This indicator is used to assess whether cancer cells have spread to other distant organs in the body.
| M Classification | Description |
| M0 | No evidence of distant metastasis. |
| M1 | Cancer cells have spread to distant organs, such as the bones, lungs, liver, or brain. |
Correlation Between Breast Cancer Staging and Survival Rates
Based on TNM classification, breast cancer is divided into stages 0 to IV, which are directly related to treatment strategies and prognosis. In general, the earlier the stage, the higher the relative five‑year survival rate.
|
Stage |
Tumor size and metastasis status |
Average five‑year relative survival rate |
|
Stage 0 |
Non‑invasive cancer: Cancer cells have not invaded other tissues. |
99% |
|
Stage I |
Early invasive cancer: Tumor is less than 2 cm and has not spread to the axillary lymph nodes. |
99.3% |
|
Stage II |
Invasive cancer: Tumor size between 2–5 cm, possibly spread to nearby lymph nodes. |
94.6% |
|
Stage III |
Locally advanced invasive cancer: Tumor is larger than 5 cm, has invaded the skin, or has spread to multiple lymph nodes. |
76.2% |
|
Stage IV |
Metastatic cancer: Cancer has spread or metastasized to distant sites. |
29.8% |
Preparation Before Treatment
- Maintain healthy lifestyle habits, including a balanced diet and regular routines, without making drastic changes.
- Inform the anesthesiologist of any drug allergies and the medications you are currently taking.
- Consult your doctor about possible post‑surgery complications and how they can be managed.
Treatment Methods
The treatment and prognosis for breast cancer depend on staging of breast cancer. Physicians will recommend treatment options based on the staging and types of breast cancer. The main treatment approaches include the following: upfront surgery, neoadjuvant treatment, i.e. use of chemotherapy, targeted therapy, hormone therapy, and/or immunotherapy before operation, and adjuvant treatment i.e. use of chemotherapy, radiotherapy, hormonal therapy after operation.
Surgical Resection
- Surgical resection includes:
- Breast-conserving surgery
- If the tumor is relatively small, the surgeon will remove the tumor along with surrounding tissue, followed by radiotherapy.
- Total mastectomy
- If the breast lump is large or when patient is not suitable for radiotherapy, the entire breast needs to be removed.
- Sentinel lymph node biopsy
- This procedure involves removing the sentinel lymph node and analyzing it to determine whether cancer cells are present. The sentinel lymph node refers to the first (few) lymph node(s) in the axilla; when cancer cells spread from the breast tumor into the lymphatic system, they typically accumulate in the sentinel node before spreading to other axillary lymph nodes.
- Breast-conserving surgery
Chemotherapy
Chemotherapy uses anti‑cancer drugs to destroy or suppress cancer cells in the body. Treatment courses generally last about three to six months. It could be administered as neoadjuvant therapy before operation or adjuvant therapy after surgery to reduce the risk of recurrence.
Radiotherapy
Radiotherapy uses ionizing radiation to kill cancer cells. The radiation damages cancer cells at the genetic level, preventing them from reproducing. Treatment courses generally last about three to four weeks. Radiotherapy is often combined with surgery and chemotherapy to enhance effectiveness and reduce the risk of recurrence.
Immunotherapy
Immunotherapy uses own immune system’s cells fight against cancer cells.
Targeted Therapy
Targeted therapy uses drugs to selectively attack cancer cells. It is designed to enhance the effectiveness of chemotherapy and is particularly effective for HER2‑positive breast cancer. The treatment course typically lasts about one to one and a half years.
| Targeted Therapy Regimen | Main Drug(s) | Common Treatment Approach |
| HER2 Breast Cancer Treatment Regimen | Trastuzumab Pertuzumab | Combined with chemotherapy |
| Luminal (Hormone Receptor‑Positive) Breast | CDK4/6 Inhibitors | Combined with hormone therapy |
Hormone Therapy
Hormone therapy involves taking anti‑estrogen medications to prevent cancer cell growth. It is suitable for patients whose tumors show a positive hormone receptor response, and may also be used as treatment following chemotherapy. The duration of therapy varies by individual and can last up to 5-10 years.
| Type of Hormone Therapy | Eligible Patients | Main Medications | Number of doses |
| Antiestrogen therapy | Premenopausal and postmenopausal women | Tamoxifen | Oral administration once daily, treatment course approximately 5–10 years |
| Aromatase inhibitor therapy | Postmenopausal women | Anastrozole、Letrozole & Exemestane | Oral administration once daily, treatment course of 5 years or longer |
| Ovarian function suppression therapy | Premenopausal women | Goserelin | The medication suppresses ovarian estrogen production. When treatment stops, the ovaries resume estrogen production. |
Breast cancer treatment choices are complex decisions. If you have any questions, you should consult your doctor as soon as possible. For professional advice, you may contact the Breast Surgery at Hong Kong Adventist Hospital.
Postoperative Care and Rehabilitation After Breast Cancer Surgery
- Physical care:
- Arm exercises: Use exercise bands to perform stretching movements of the upper arm to help prevent postoperative lymphedema and restricted shoulder movement.
- Physiotherapy: Breast cancer surgery or radiotherapy may damage lymph nodes. Early physiotherapy, such as exercise and lymphatic drainage, can reduce the risk of lymphedema after axillary lymph node removal and restricted shoulder movement.
- Balanced nutrition: Adjust lifestyle and diet to promote recovery.
- Psychological care:
- Emotional support: Seek encouragement from partners, family, friends, and support groups.
- Regular follow‑up: Attend scheduled medical reviews to regain normal life.
How to Prevent Breast Cancer and Understand the Risk of Recurrence
To effectively prevent breast cancer, it is important to exercise regularly, maintain a balanced diet, and keep a healthy body weight and waist circumference. In addition, avoid excessive alcohol consumption and develop good habits such as regular breast check‑ups.
The risk of breast cancer recurrence is highest within the first five years, particularly during the first one to two years. However, even after five years, a certain proportion of patients may still experience recurrence after ten years.
FAQ About Breast Cancer
Does a breast cancer diagnosis always require total mastectomy?
Not necessarily. The decision depends on factors such as the size, location, and extent of the tumor, as well as the proportion of breast volume, and will be determined after medical evaluation.
Why is adjuvant chemotherapy or targeted therapy needed after breast cancer surgery?
It is primarily to eliminate microscopic cancer cells that cannot be completely removed by surgery, thereby preventing recurrence or metastasis and increasing the chances of cure.
Is breast size related to the causes of breast cancer?
Breast size is not related to the causes of breast cancer, but high breast density increases the risk of developing the disease.